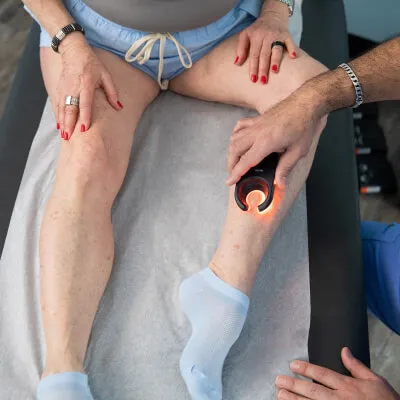
Knowing how to prevent blood clots means understanding risk factors: that is, why they happen in the first place. Here, we'll explain all about blood clots, deep vein thrombosis, and pulmonary embolism--and tell you what you can do to avoid experiencing a life-threatening emergency like a heart attack or stroke.
How to Prevent Blood Clots
Blood clots are actually a normal part of our body functions (as an example, to stop bleeding), but if blood clots in the wrong place at the wrong time, it can be very serious. Luckily, there are ways to help prevent these unhealthy blood clots from happening in the first place.
How Common are Blood Clots?
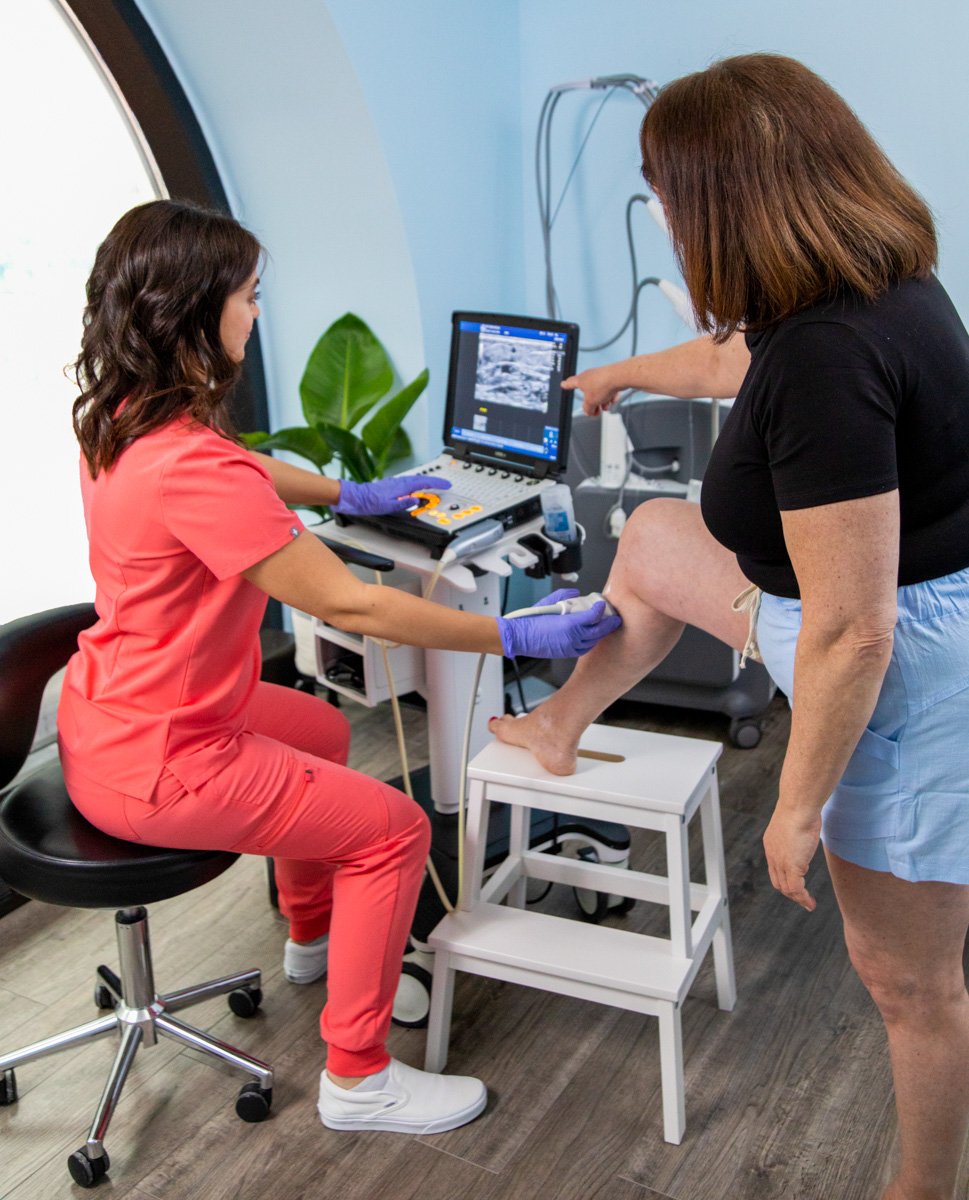
Blood clots are more common in those aged 60-80, but people of any age can get one. In fact, blood clots are one of the biggest, yet preventable, causes of hospital deaths in the USA. About one in every 10 hospital deaths is related to blood clots in the lungs. So how common are clots? Common enough that everyone should understand risk factors and be aware of potential symptoms so they can know what to look out for.
Who Gets Blood Clots? Am I at Risk?
The best ways to prevent getting blood clots is to keep yourself in good health, know your risk factors, and seek out a vein and vascular specialist if you have any of the common blog clot symptoms discussed below.

Blood clots can affect anyone, no matter their age, gender, or race. Even a fit 40-year-old woman recovering from knee surgery could be at risk, just as a 75-year-old man who is confined to a wheelchair could be. Certain factors make bigger impacts than others, though, so it's important to know what to look for.
You could be at extra risk for blood clots if you:
- have just had major surgery, such as replacements of your hips or parts of your legs
- smoke
- fly for long periods of time or sit for long periods of time
- are over the age of 50
- take certain types of treatments that contain estrogen
- suffer from chronic diseases such as diabetes, cancer, or heart conditions
- are severely overweight
- have been hospitalized and are immobile
Blood Clot Symptoms
Correctly diagnosing any possible blood clot symptoms or pains in your body is a job only for specialty doctors trained to evaluate vein and vascular conditions, but it's also important to know any warning signs so you can know when to seek medical attention.
Blood clot symptoms and warning signs include:
- shortness of breath
- swelling, especially in your legs and arms
- skin discoloration, typically a reddening or darkening of the skin
- tender or warm skin
In contrast, those who are experiencing a pulmonary embolism may experience:
- intense abdominal pain
- coughing up blood
- extreme shortness of breath and difficulty breathing
- fainting spells
- irregular heartbeat
See a doctor right away if you experience these symptoms.
What's a Blood Clot vs Deep Vein Thrombosis vs Pulmonary Embolism?
There's a lot of confusing lingo when it comes to blood clots and related health concerns: thrombosis vs embolism; blood clot in the legs or lungs. Let's set the record straight!
A deep vein thrombosis and a pulmonary embolism are both types of blood clots.
Both can be dangerous.
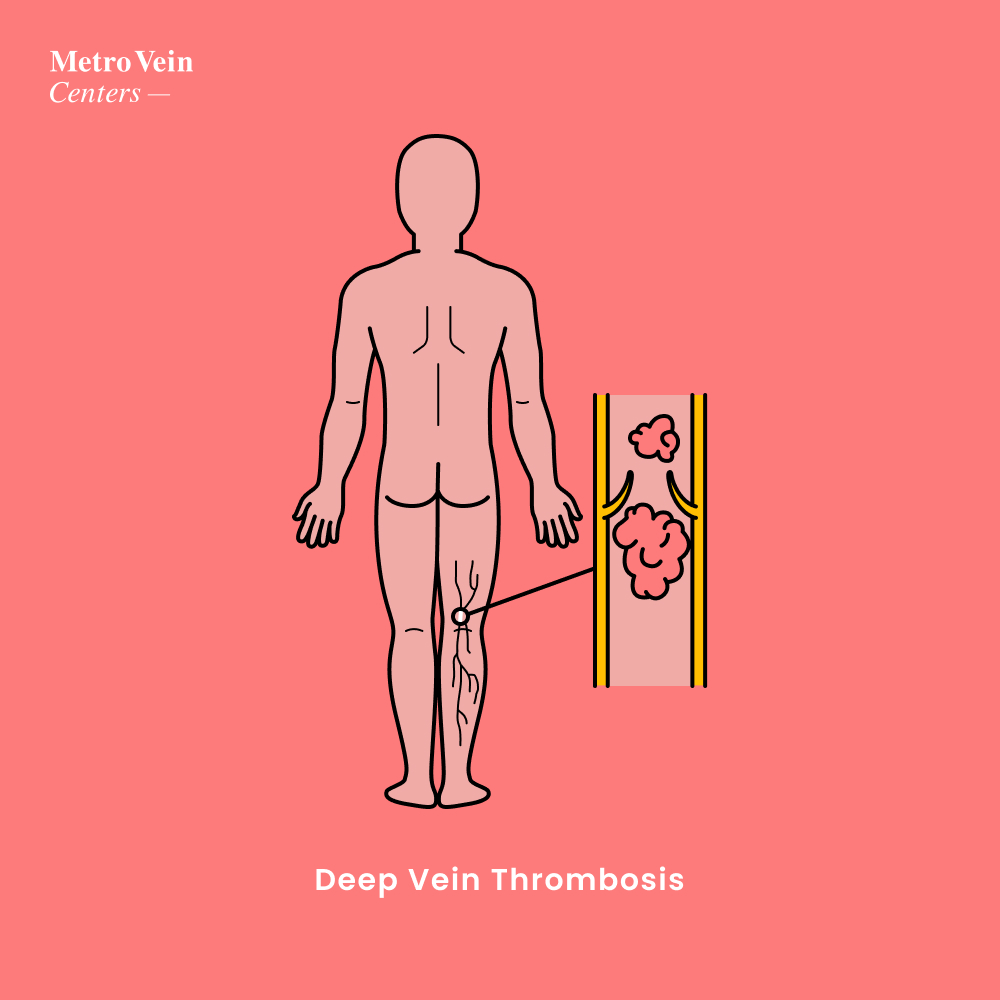
Deep Vein Thrombosis, otherwise known as DVT, is a type of blood clot that forms in the leg, or, in rare cases, around the hips or arms. Most cases of deep vein thrombosis occur when a clot breaks off in a leg vein, constricting the vein and thus preventing the blood from properly cycling through your body.
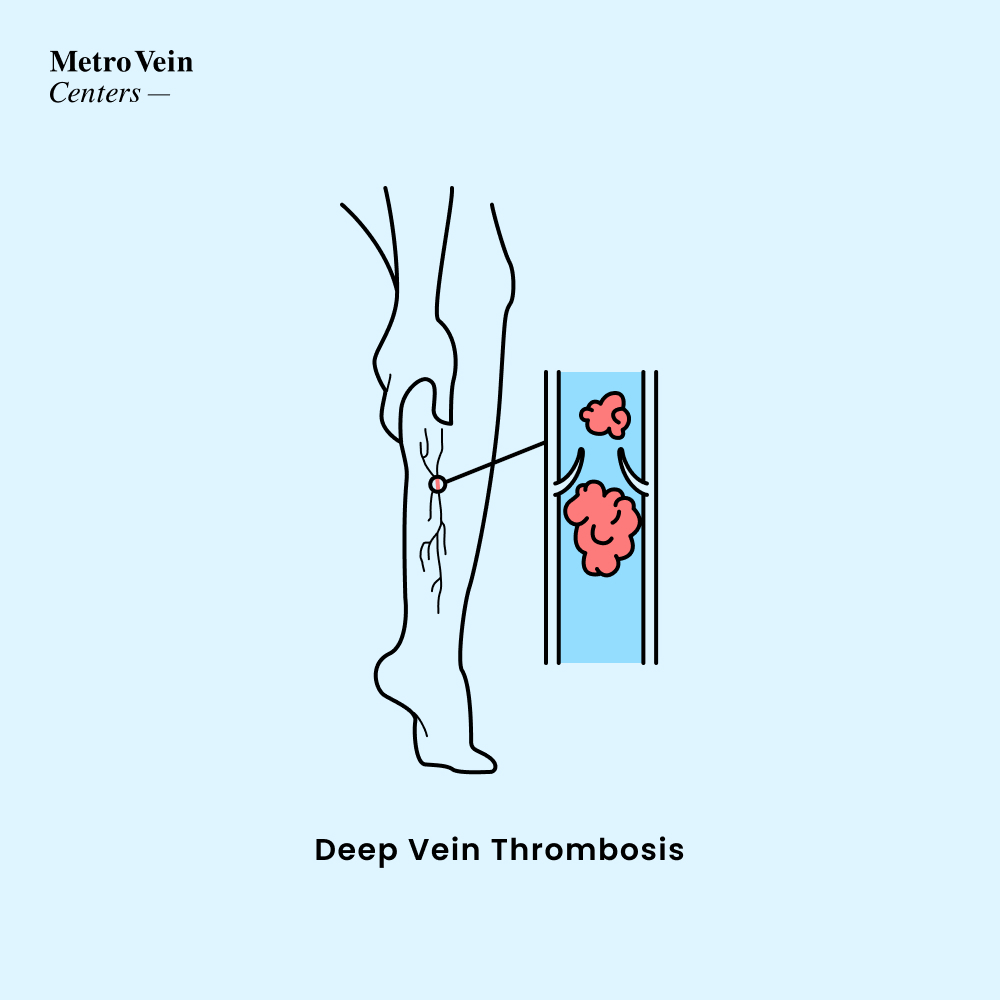
Pulmonary Embolism is a condition where a blood clot travels up into the heart and then lungs, completely blocking blood flow. A pulmonary embolism, or PE for short, is caused when a deep vein thrombosis is not treated. A PE can cause death, and needs to be taken very seriously. Acute embolisms have death rates as high as 30%, but when treated preventatively or immediately, that rate can be cut down to just a small number.
People with poor vein circulation and those with venous insufficiency are more at risk for a deep vein thrombosis--and, by association, a pulmonary embolism. Why? Patients with damaged veins are more likely to link pain with movement, and people at risk for blood clots are often those who don't move around much. It's a dangerous catch-22.
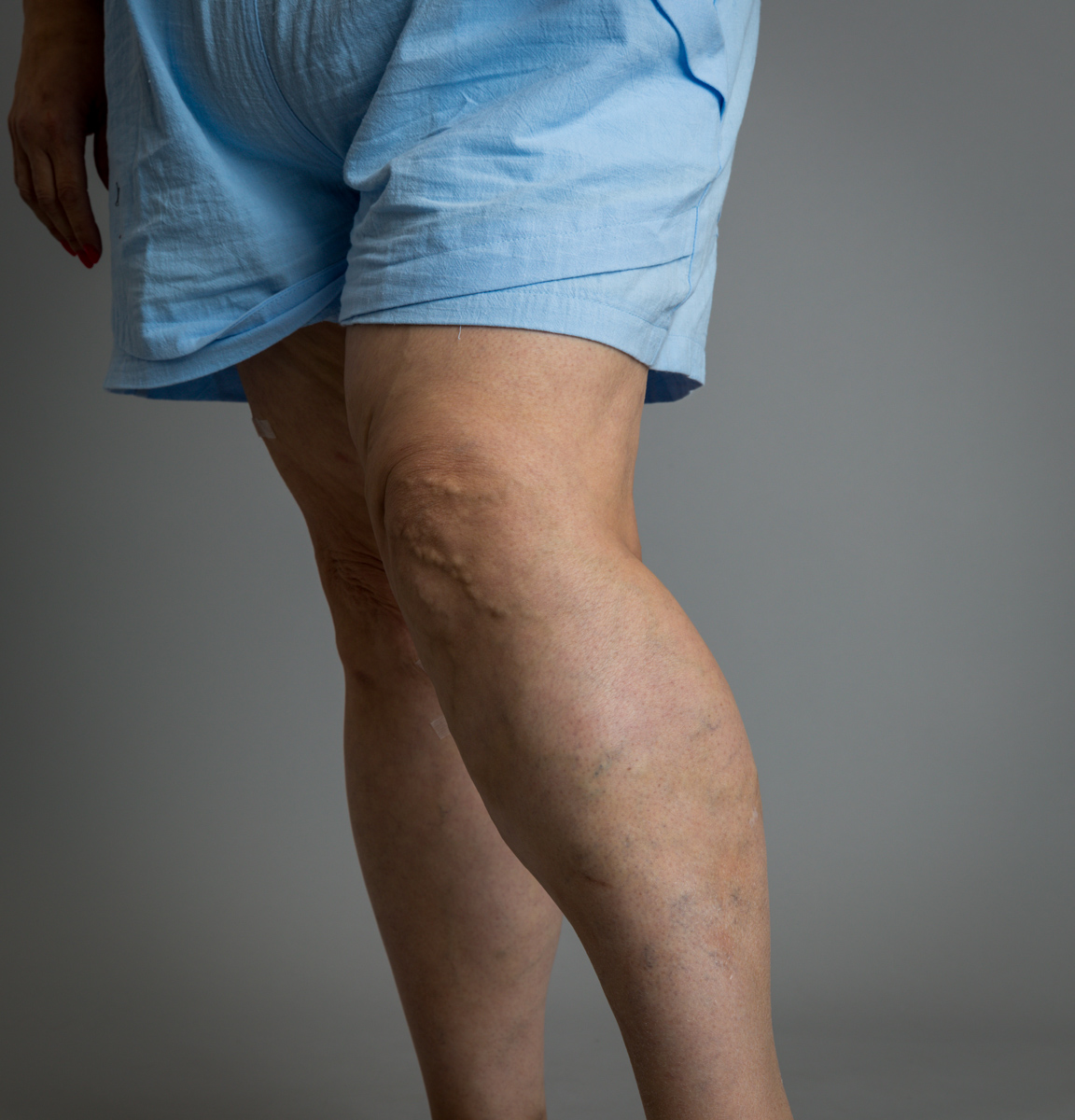
What Can I Do to Prevent Blood Clots?
Certain risk factors that raise your chances of getting a blood clot are preventable. Maintaining a healthy weight, exercising, and being aware of blood clot symptoms and signs are the best ways to stay on top of any blood clot warnings. Stress, anxiety attacks, and constant worry can actually make your chances of getting a blood clot worse, so scheduling a consultation with a vein specialist at Metro Vein Centers who can evaluate your vascular system is the smartest way to get answers and peace of mind.
Here's what we recommend you do to avoid and prevent blood clots that could be life-threatening:
- Monitor your weight and do your best to maintain a healthy BMI.
- If sitting or laying down all day, stand up frequently to stretch and move the legs around.
- Know your family history: Understand if family members have suffered from blood clots.
- Surgery? Know your risks going in, and make sure you're well monitored post-surgery.
- Wear compression stockings to promote circulation.
- Exercise when you can, even if it's just a 10-minute walk to get you out of a chair.
- Get an ultrasound and/or blood tests from a licensed vein specialist.

Blood clot prevention means knowing your risks, moving frequently, and being proactive
The best way to prevent blood clots is to take care of your body, find out your family history, and visit a vein specialist. At your Metro Vein Centers appointment, we'll do a pain-free scan of your legs to find out what's visible and underneath the surface of your skin. When it comes to blood clots, knowledge and action is the best prevention of all.
Book your Metro Veins Centers appointment today!
Fill out our 4-question form: Click here Or, call us: 888-660-3494
Metro Vein Centers Editorial Team
From vein care 101 to treatments, the Metro Vein Centers blog offers patients everything they need to know about vein health.

Trusted insight from the nationally accredited, board-certified vein doctors at Metro Vein Centers.