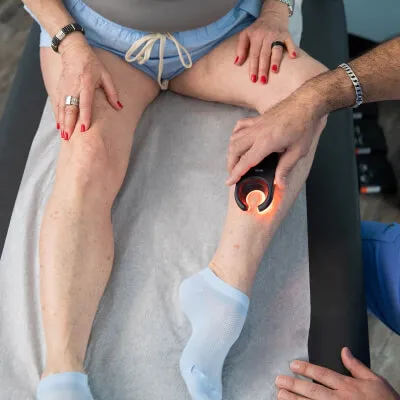
Deep vein thrombosis, or “DVT,” is a medical condition that often occurs in the legs when blood clots form in veins deep beneath the surface of the skin. What are the risk factors for DVT? Does everyone with varicose veins develop DVT? What can we do to prevent blood clots from forming? Let’s dive in!
Why Is DVT So Dangerous?
DVT is dangerous because blood clots can cause serious and life-threatening issues when they break off from the inside of a deep vein and travel through the circulatory system. While stuck to the wall of a deep vein, blood clots will slow your blood flow and negatively impact your circulation, which can also worsen the symptoms of vein disease. When they travel, immediate emergency care is required. Understanding blood clots is key to understanding DVT.
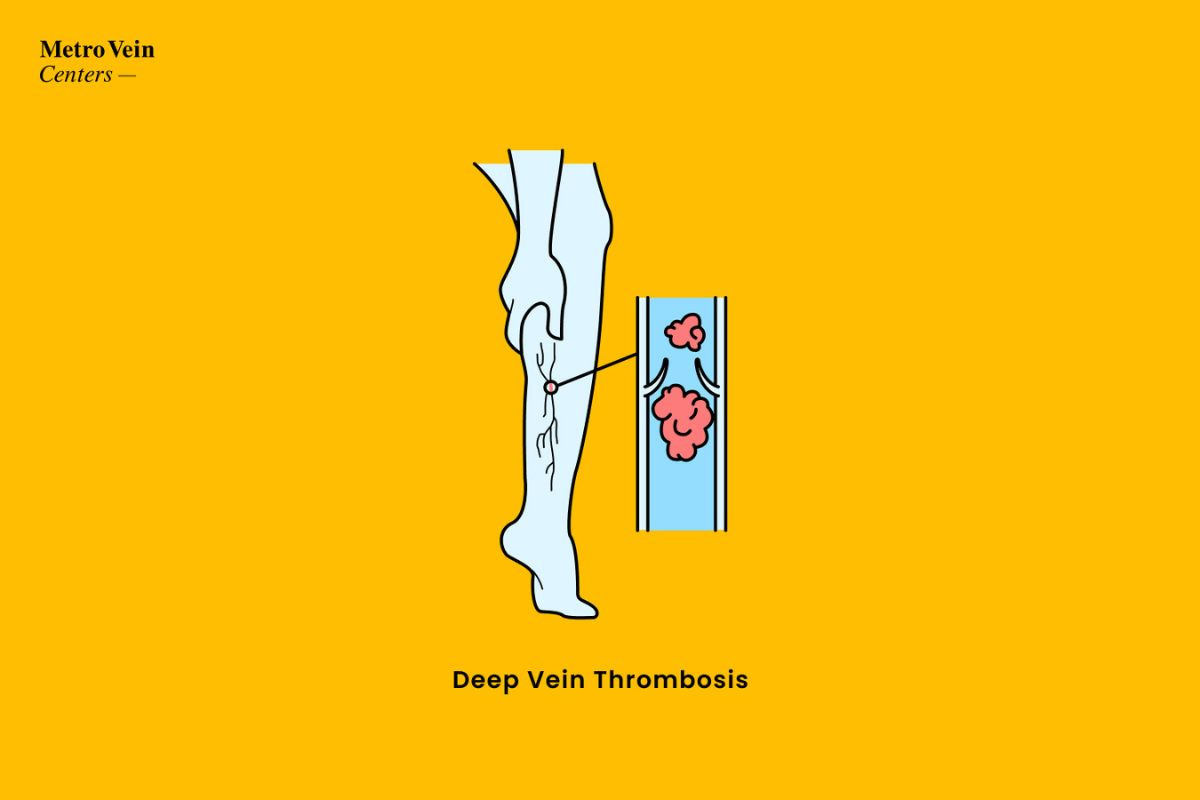
Anatomy of Deep Veins
Your deep veins, like veins closer to the surface, have structures (aka vein valves) on their interior that operate like water-tight doors. The function of a venous valve is to keep blood flowing and prevent blood from becoming stagnant or pooling. When blood pools, it results in venous stasis, and veins have more and more trouble effectively pumping blood back to the heart. In diseased veins, these valves often malfunction and cause blood to accumulate in areas where the vein has become warped.
Deep vein thrombosis occurs when there is a blood clot in the deep system that may cause complete obstruction of blood flow leading to generalized leg warmth, redness, pain and swelling. If dislodged, it can lead to life-threatening complications such as a pulmonary embolism. In surface veins, blood clots are rarely life-threatening, but can still cause uncomfortable symptoms like skin discoloration, warmth, pain, and swelling in the affected area. In surface veins, it’s easier to tell if they’ve become diseased as they may appear as twisted, cord-like varicose veins that are visible to the naked eye. In deep vein systems, usually we cannot see visible symptoms due to the depth of the affected veins. Therefore, superficial thrombosis is often caught, and deep vein thrombosis may fly under our radar longer.
Poor circulation is an uncomfortable side effect, but the real risk is a bit more concerning: Because your veins carry blood back to your heart and lungs to be re-oxygenated, blood clots in veins can easily travel toward these critical organs once they detach from a vein wall. When blood clots break free from deep veins, they travel with the flow of blood back toward the circulatory system’s center. If they lodge in the lungs, a patient can experience a pulmonary embolism.
Pulmonary embolism is a serious, often life-threatening condition that requires emergency care. If blood clots become trapped in the arteries of the lungs, they can cause damage, shortness of breath, decreased oxygen in the body, and death. Because the lungs re-oxygenate your blood and keep your body functional, if a clot from DVT has obstructed your blood’s oxygen source, your circulatory system is unable to perform its most important function: moving your blood around.
The goal of your vein doctor in diagnosing deep vein thrombosis is to treat your venous concerns before the blood clots have the chance to become embolisms. Luckily, DVT is a highly treatable condition, and although pulmonary embolism is a late-stage side effect, it is not the only outcome of a DVT diagnosis.
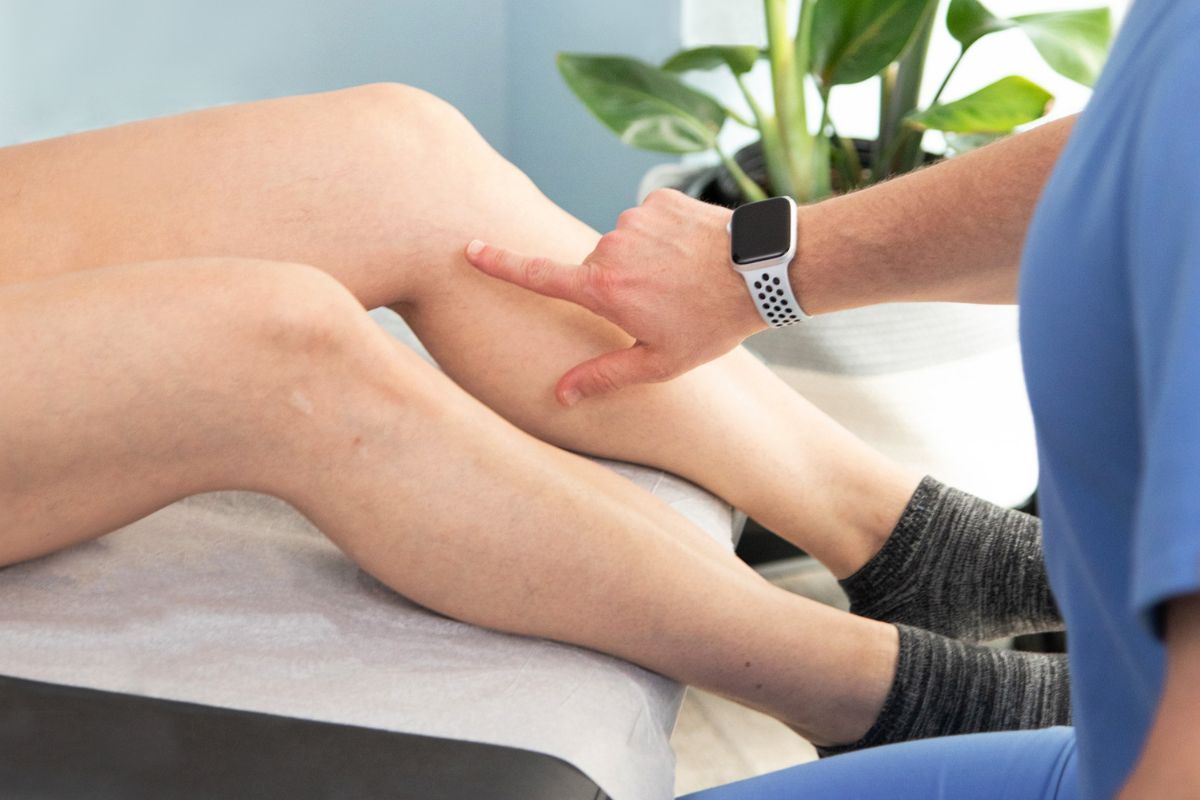
How Does DVT Develop?
DVT is most likely to occur in veins on the lower legs and pelvic region; these veins have a hard job of working against gravity to bring blood back to the heart from our lowest extremities, so these veins are more likely to develop venous insufficiencies. Varicose veins, a result of venous insufficiency, occur on the surface of the skin and are easy to identify because they are often visibly bulging, twisted, and easy to see. Venous insufficiency can also occur deeper beneath the skin, in veins surrounded by muscle and far enough away from the surface that they cannot be seen or monitored by the naked eye. It is within these deep veins that DVT can develop and endanger the health of someone suffering from vein disease.

Understanding the Causes and Risk Factors For DVT
Like with other venous insufficiencies, DVT has many common risk factors, some of which are affected by lifestyle choices and some that are outside of our control. It’s important to remember that (like with varicose veins) we will never be able to fully prevent DVT. However, understanding risks helps us to prepare, monitor, and treat symptoms of vein disease and DVT.
Some risk factors include:
· Age: Deep vein thrombosis, like a surface vein blood clot, can occur at any age. However, the likelihood of developing DVT begins to increase in patients over 60 years old.
· Smoking or tobacco use: Nicotine can cause platelets in your blood to become stickier, which makes it easier for clots to form.
· Obesity: Excess weight puts more pressure on the veins, leading to venous insufficiencies and vein diseases which can increase the chance of developing DVT.
· Pregnancy/Postpartum: Pregnancy creates a hypercoagulable state, which helps prevent postpartum bleeding, but also creates an environment that may increase risk of clot formation. Postpartum varicose veins are very common.
· Sedentary lifestyles: Regular exercise and movement increases blood circulation, whereas little movement and poor circulation can lead to blood clots.

· Frequent air travel: If you often travel at long stretches and don’t take the time to move around (flex your feet, walk, or stretch), your risk of developing blood clots increases.
· Surgeries, specifically joint replacements: Any surgery or injury to the vein increases risk of DVT. In addition, patients undergoing hip, knee, or other joint-replacement surgeries are at a higher risk for DVT because mobility can be limited during recovery.
· Birth control: Blood clots are a common side effect of estrogen birth control pills.
· Varicose veins: Diseased veins are at a higher risk of trapping blood clots. In varicose veins, the walls are weakened and twisted, circulation is decreased, and blood is more likely to stick together and form a clot.
· Genetics: If you or a family member has a medical history of a clotting disorder, blood clots, or vein disease, your risk increases.
· Inflammatory bowel disease (IBD): Crohn’s and other inflammatory bowel diseases activate a clotting cascade, leading to an increased risk of developing clots.
Did you know? DVT affects 1 to 3 of every 1,000 people!
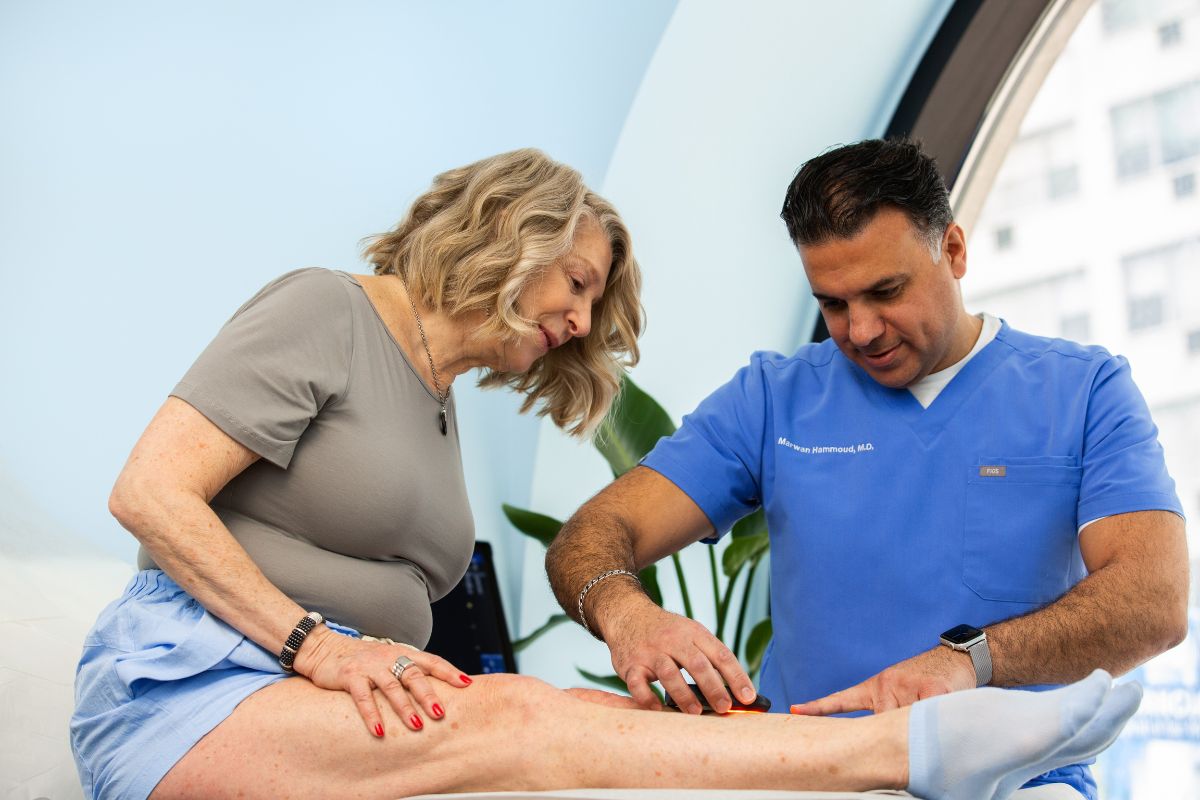
The Signs and Symptoms of DVT
When diagnosing DVT, there are four primary symptoms your vein doctor will check for. These typically present in only one leg at a time.
· Leg swelling
· Unexplained leg pain
· Reddened and skin warm to the touch
· Hard veins under the skin
DVTs are often painful or uncomfortable, but can also be symptomless, depending on the stage of the DVT. Your vein doctor will ask what sensations you are experiencing and then perform an ultrasound to diagnose your condition. If you notice you have visible swelling, new discoloration, or warm skin in only one of your legs, you should book an appointment with your vein doctor right away or seek urgent care, as these could be signs of an acute DVT.
DVTs are serious and, if left untreated, they put you at risk of pulmonary embolism, which can be fatal. Our team at Metro Vein Centers can help to rule out a serious complication and identify whether your symptoms are a result of DVT or other forms of venous insufficiency.
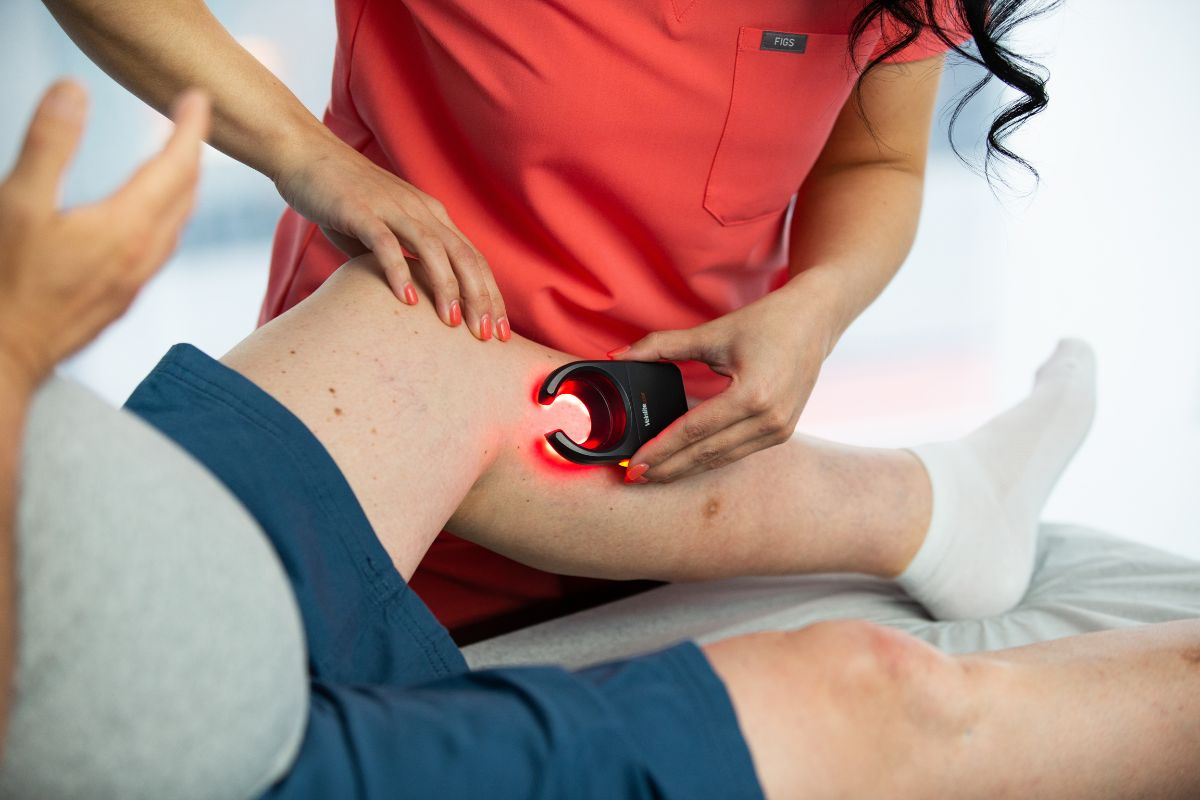
How We Treat Deep Vein Thrombosis
Following your consultation and ultrasound evaluation, our board-certified vein specialists will identify whether you are experiencing deep vein thrombosis or another form of vein disease. We highly recommend seeking urgent or emergency care if you suspect you are experiencing symptoms of vein disease and/or deep vein thrombosis because these conditions are progressive (meaning they can only get worse with time, if left untreated). We always recommend seeking medical attention if you start to notice changes in your legs.
Although we do not treat emergency cases of DVT in our vein clinics, there are treatment options available for those who have been diagnosed with DVT via ultrasound evaluation. Anticoagulant medication (either oral or non-oral medications) as prescribed by your physician can assist in the dissolution of blood clots. Anticoagulants do not dissolve the clot; they prevent the body from making clots worse so that the body has an opportunity to break down the clots and heal itself. (This process can take days or weeks.) Compression stockings are often prescribed to promote healing and good circulation in the legs while they are being treated. In severe cases, or when the risk of pulmonary embolism is high, surgical intervention may be necessary.

What to Do and What Not to Do
Following your diagnosis of DVT, your vein doctor may recommend you do some of the following at home:
DO
· Take your blood thinners, if prescribed by your doctor
· Wear your compression stockings to relieve swelling or pain, and help with the healing process
· Light exercisesuch as gentle walking, is a great way to safely engage your leg muscles and promote good blood flow.
· Invest in healthier lifestyle choices. Eating a well-rounded diet, quitting smoking, and maintaining a healthy weight will all decrease your risk of developing DVT and vein disease in the future.
· Elevate the affected leg to improve circulation.
· Schedule a follow-up visit with your vein doctor.
· Take our Vein Health Quiz to better understand your symptoms.
DO NOT
· Massage the affected leg. This can dislodge blood clots adhered to the vein wall, increasing risk of the blood clot traveling to the lungs and becoming a pulmonary embolism.
· Ignore your symptoms. Pulmonary embolism is an extremely dangerous condition, and DVT must be taken seriously in order to avoid blood clots migrating.
At Metro Vein Centers, we treat all forms of vein disease - from cosmetic spider veins to varicose veins. If you are concerned about your symptoms or are curious about the health of your veins, our board-certified vein doctors are here to help! We accept more than 200 insurance plans, and over 97% of our vein treatments are covered by insurance! We’ll work with you to make sure your treatments are covered. Our goal is to deliver the highest quality, customized care to all our patients. We treat your unique symptoms with state-of-the-art technology and offer minimally invasive procedures to ensure that your health and comfort come first.
We look forward to seeing you in one of our New York, New Jersey, Michigan, Connecticut, Pennsylvania, Arizona, and Texas vein clinics!

Dr. Philip LoPresti
Meet Dr. Philip LoPresti DO, DABVLM, FACS, a board-certified vein specialist and surgeon with over 20 years of experience. Schedule an appointment with him in Queens, NY today.
Meet Dr. Philip LoPresti
Trusted insight from the nationally accredited, board-certified vein doctors at Metro Vein Centers.