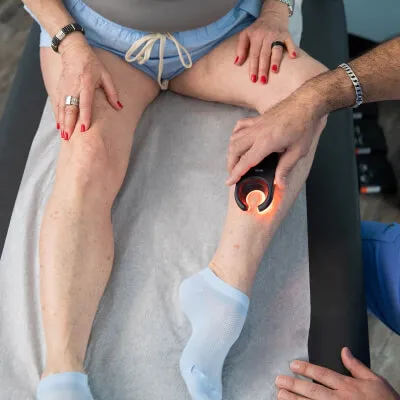
Varicose veins and spider veins are a very common condition affecting 1 in 3 men and 1 in 2 women over the course of our lives. In some cases, varicose veins can be a mere cosmetic concern; however, they are most often indicative of an underlying medical condition known as Chronic Venous Insufficiency (aka “Vein Disease”) which can cause pain while standing, itching/tingling, swelling, aching, and even restless legs.
Can You Get Rid of Varicose Veins at Home?
No, you can't completely get rid of varicose veins at home, but self-care methods can help alleviate symptoms. Regular exercise, maintaining a healthy weight, elevating your legs, wearing compression stockings, and avoiding prolonged standing or sitting can prevent worsening.
For significant improvement, medical treatments like sclerotherapy or laser therapy are needed. Consult a healthcare professional for proper diagnosis and treatment.
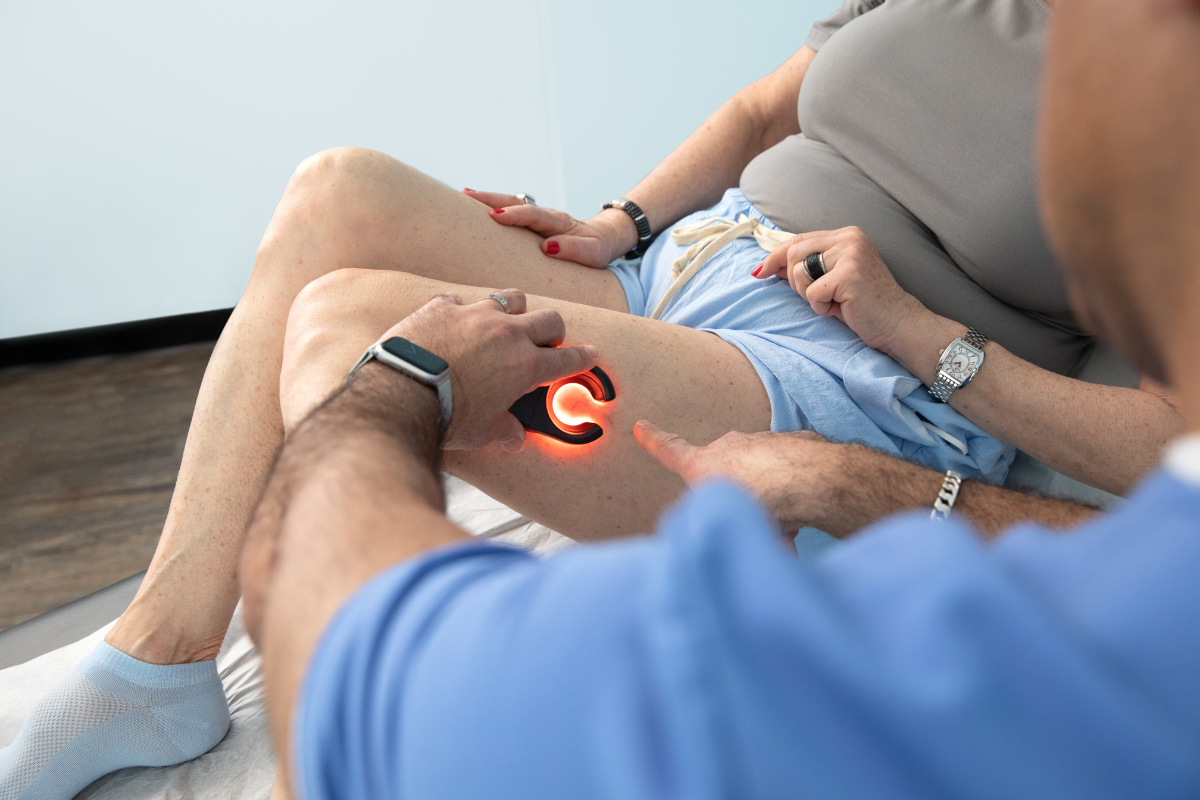
Understanding Varicose Veins
Varicose veins on the legs can be identified by their swollen, twisted appearance, often slightly raised above the skin. These veins appear most often on the thighs and calves and can cause pain, itching, and discomfort. They occur when the valves in the veins become weak and don't function properly, leading to blood pooling in the legs, backward-flowing blood, and other circulation issues. When blood pools in the veins and circulation is negatively impacted, this can affect your overall health and quality of life. Several factors contribute to the development of varicose veins, including genetics, age, sex/gender, family history, and more.
At-Home Remedies Cannot “Cure” Varicose Veins, But They May Temporarily Relieve Pain
While the underlying medical condition of Chronic Venous Insufficiency cannot be cured without medical intervention through minimally invasive vein treatments, some patients seek relief from mild symptoms using at-home remedies and lifestyle changes while they research their options and consider pursuing vein treatment. At-home remedies are DIY ways that you can improve your circulation and work to help the damaged valves in your veins. These methods act with a goal of restoring (or aiding) proper blood flow, which in turn can temporarily relieve the pain and/or discomfort commonly associated with pesky varicose veins.

10 Tips from our Vein Specialists To Try at Home
1. Compression Therapy:
Over-the-knee compression stockings are designed to provide graduated pressure on the legs, helping to push blood upward and reduce swelling. These stockings can significantly improve blood circulation and alleviate varicose vein symptoms. To achieve the best results, choose thigh-high, medical-grade compression stockings in a size appropriate for your height, such as those from Ames Walker, which provide enough compression to achieve a significant improvement in blood flow. Our vein specialists recommend stockings with at least 20-30 mmHg of compression strength for the best results.
2. Elevate Your Legs:
Elevating your legs is a simple yet effective way to relieve pressure on your veins and improve blood flow. When sitting or lying down, prop your legs up with pillows to encourage better circulation. A lot of the issues we see from varicose veins are due to valves malfunctioning, causing blood to flow in the wrong direction, toward your feet. Propping your legs up encourages blood to flow in the right direction back to your heart. We recommend at least 30 minutes of comfortable elevation at the end of the day to maximize the benefits of leg elevation.

3. Stay Active:
Regular, low-impact exercise can play a crucial role in improving blood circulation and preventing blood from pooling in the veins. Engaging in activities such as walking, swimming, and yoga for at least 30 minutes each day can help keep your veins healthy and reduce the risk of varicose veins. Learn more about exercise and vein health here.
4. Maintain a Healthy Weight:
Excess weight and the strain of gravity can put additional pressure on your veins, contributing to the development of varicose veins. A balanced, diverse diet and incorporating these food groups into your meals can help you maintain a healthy weight, reducing the strain on your veins and promoting overall vascular health.
5. Hydration
Staying well-hydrated is essential for maintaining healthy blood circulation. Avoiding excess caffeine, alcohol, and other dehydrating beverages, which cause the veins to contract, in favor of consuming more water can help your overall bodily health as well as improve the blood flow in your veins.

6. Avoid Prolonged Sitting and Standing:
Long periods of inactivity, whether sitting or standing, can negatively impact blood circulation. If you have a desk job or are in a car for long periods of time, make an effort to take short breaks to stretch and move around (compression socks can help!). For those who stand for extended periods, shift your weight from one leg to the other, stretch, and take seated breaks when possible.
7. Massage Your Legs:
Gentle massage can help improve blood flow and alleviate discomfort in your legs. Use your fingertips and a skin lubrication such as oil or lotion to apply gentle pressure and move in upward motions along your legs. A light massage followed by leg elevation is recommended by our vein specialists as a way to get a double-dose of benefits to improve circulation at home.
8. Avoid Tight Clothing
While they may seem similar to compression stockings, tightly fitted clothes such as Spanx, elastic socks, and skinny jeans can actually restrict circulation in the legs and lead to blood pooling. In addition, while it is a myth that high heels can cause varicose veins, wearing them for prolonged periods of time can result in painful swelling or aching in the legs due to lack of circulation. For this reason, we recommend avoiding high heels if you are experiencing painful varicose veins or aching, heavy legs.

9. Use Over-the-Counter Pain Relievers (Temporarily)
While we do not recommend over-the-counter pain relief as a permanent solution to ongoing discomfort and leg pain, temporary pain and swelling may be alleviated by using over-the-counter remedies such as Tylonol or Ibuprofen.
10. Avoid Ineffective Therapies
While it is tempting to try to handle every aspect of your vein concerns from home, we advise against ordering at-home “medical equipment” from sources not affiliated or endorsed by the FDA. This includes using vein “firming” creams and oils, or “blue light pens” being sold online or in non-accredited medspas. These are not proven to have any impact on spider veins or varicose veins.
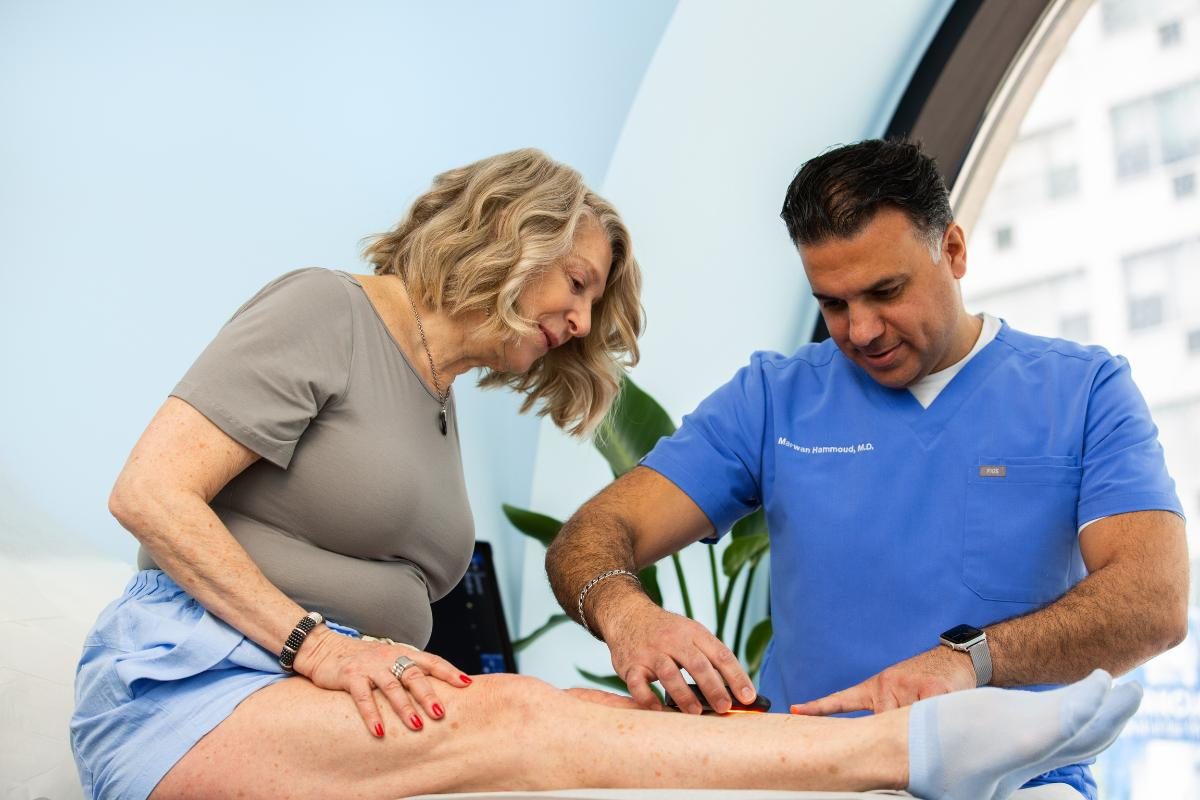
When to Seek Advice from a Vein Specialist:
While home remedies can provide short-term relief, it is essential to consult a healthcare professional if symptoms do not improve or if your attempts at finding meaningful relief only provide a temporary reprieve. Vein disease is a progressive condition, and the broken, leaky valves that cause visible varicose veins will not go away or heal themselves without medical vein treatment. It is best to seek out a board-certified vein doctor and FDA-approved vein treatment if you are looking for lasting, permanent relief (which, we hope you are! No pain is normal, and you deserve to have healthy, happy legs).
If you experience any of the following symptoms, you should contact a vein specialist immediately as these symptoms could be signs of serious blood clot or Deep Vein Thrombosis: sudden and/or asymmetrical changes in leg swelling, unexplained throbbing leg pain, skin that is flushed and/or warm to the touch, or hard veins under the skin.
Where Can I Go To Get Vein Treatment Near Me?
At Metro Vein Centers, we treat all forms of vein disease and vein care concerns - from cosmetic spider veins to more advanced stages of chronic venous insufficiency such as varicose veins, edema, and ulcers. If you are concerned about your symptoms, are experiencing discomfort, or if you are curious about the health of your veins, our board-certified vein doctors are here to help! We accept over 200 insurance plans, and over 97% of our vein treatments are covered by insurance! Our goal is to deliver the highest quality, customized care to all of our patients. We treat your unique symptoms with state-of-the-art technology and offer minimally invasive vein therapies to ensure your health and comfort comes first. Healthy legs feel better! Our patient care team is available to answer any questions and get you started with your free vein evaluation at 866-353-4952.
We look forward to seeing you in one of our New York, New Jersey, Michigan, Connecticut, Texas, Arizona, and Pennsylvania vein clinics!

Metro Vein Centers Editorial Team
From vein care 101 to treatments, the Metro Vein Centers blog offers patients everything they need to know about vein health.

Trusted insight from the nationally accredited, board-certified vein doctors at Metro Vein Centers.