The Quick Answer
Chronic stress can directly impact your leg veins. Prolonged stress keeps your blood pressure elevated and releases inflammatory hormones like cortisol, both of which can weaken vein walls over time and worsen symptoms of vein disease.
You don't have to wait until National Stress Awareness Day in November to think about what chronic stress is doing to your vein health. We know that stress impacts our sleep, mood, and even blood pressure. But did you know that chronic stress can also take a heavy toll on your leg veins?
While we tend to think of vein issues as purely medical or genetic, your emotional well-being can play a surprising role in your vascular health. Let's explore how chronic stress can cause negative changes to your circulation, why it happens, and what you can do to protect your legs.
What Is Chronic Stress and Why Does It Matter for Veins?
To understand how stress affects your vascular system, it is helpful first to discuss the difference between acute and chronic stress.
- Acute stress: Acute stress is short-term and is usually associated with a specific stressful event. Once the event is over, your body typically returns to its normal, resting state.
- Chronic stress: Chronic stress is a constant, mental pressure that can last for weeks, months, or even longer. Chronic stress means your body's alarm system never shuts off, taking a physical toll on your circulatory system.
When your body is constantly flooded with stress hormones, your heart rate and blood pressure remain elevated. Over time, this sustained vascular pressure can put extra wear and tear on the delicate valves in your leg veins, making them more susceptible to stretching, leaking, and the development of chronic venous insufficiency and varicose veins.
What Happens to Your Circulation Under Stress?
When your body is under stress, it activates its "fight or flight" response. Chronic stress causes physical changes that can affect the body's systems, including your circulation. Here's how:
- Your adrenal glands release stress hormones, primarily cortisol and adrenaline.
- Adrenaline causes your heart rate and blood pressure to spike, preparing your body for action.
- Your blood vessels constrict (vasoconstriction). When this happens, your body constricts many smaller blood vessels (arterioles). This reroutes blood flow away from non-essential areas, like your skin and lower legs, and towards your major muscles and brain.
What does this mean for your veins? While this temporary shift is normal, if stress becomes ongoing and this response is triggered day in and day out, it can tax your nervous system and circulation in your lower legs.
How Does Chronic Stress Influence Leg Vein Health?
Chronic stress can negatively impact your vascular system by releasing stress hormones that constrict blood vessels, raise blood pressure, and even trigger stress-related inflammation, which can damage leg veins and weaken valves. Inflammation and chronic stress can damage these tiny valves, preventing them from closing properly.
Hypertension and high cortisol can slowly weaken and damage the elastic tissues that make up your vascular walls. Weakened walls are less able to snap back and retain their shape. Once the walls weaken and the valves fail, blood can start to pool, which can lead to conditions like:
- Venous Insufficiency: When the veins struggle to return blood efficiently.
- Varicose Veins: Large, bulging, rope-like veins.
- Spider Veins: Smaller, visible clusters of thread-like veins.
- Blood coagulation: Chronic stress can raise coagulation levels, reducing normal blood flow and increasing the risk of blood clots in the deep veins of the legs.
- Collagen degradation: Elevated levels of cortisol can break down collagen, an important connective protein.
Stress-Induced Lifestyle Changes
Stress can contribute to unhealthy methods of coping, like stress eating, increased alcohol consumption, and weight gain. Stress can also affect the quality and duration of sleep. All of these stress-related lifestyle factors can increase your risk of developing venous disease.
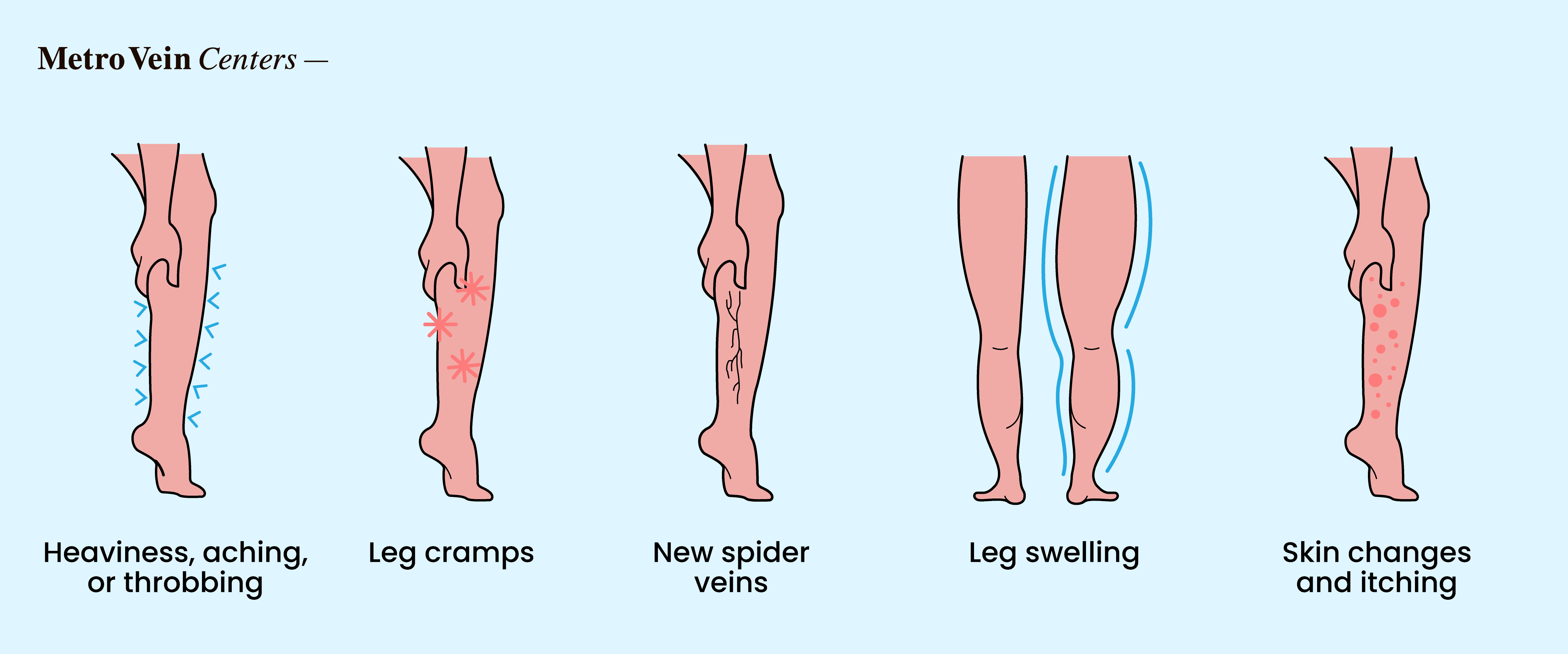
Signs That Stress Could Be Affecting Your Leg Veins
The impact of stress on your legs might show up as symptoms that you may not have connected to a vein health issue. These include:
- Leg pain, heaviness, and aching, especially at the end of a stressful day.
- Leg cramps and restless legs, particularly at night.
- Visible veins, spider veins, and varicose veins
- Leg swelling (edema) in the ankles or feet that improves overnight.
- Skin changes and itching near the veins
- Brown, purple, or darkened skin, especially around the ankles and lower calves.
Why Leg Vein Health Matters for Overall Well-Being
Ignoring early signs of vein disease isn't just a cosmetic concern; it can affect your overall health and quality of life in several ways.
Mobility and Activity
Healthy veins are essential for good circulation, which powers your muscles. Compromised veins can lead to pain, fatigue, and heaviness, making you less likely to exercise or enjoy your favorite hobbies.
Quality of Life
Vein health conditions that cause discomfort and self-consciousness can affect your mood and willingness to socialize.
Vein Disease Progression
Untreated venous disease can progress to serious medical issues like skin changes, non-healing ulcers, or, in rare cases, increase the risk of developing a Deep Vein Thrombosis (DVT). Consulting a vein specialist to discuss treatment options is the best way to avoid these complications and future medical costs.
When Should You See a Vein Specialist?
While managing stress at home is a great first step, it is important to know when lifestyle changes aren't enough. If your leg discomfort is persistent, it may be a sign of underlying vein disease that requires medical attention. You should schedule a vein health evaluation if symptoms of leg heaviness, aching, visible veins, or swelling have lasted more than a few weeks.
Don't wait for your symptoms to become a daily barrier to your mobility. Take the first step toward lighter, healthier legs and find a vein specialist near you to schedule a consultation at one of our accredited clinics.
Evidence-Based Strategies to Manage Stress and Support Leg Vein Health
With the right knowledge, you can become empowered to manage your stress levels and protect your leg health. Here are some tried-and-true strategies to reduce stress and support your leg health.
Prioritize Movement
Movement is a double-win. Low-impact exercises like walking, cycling, and swimming are great stress relievers and work the calf muscles, which are crucial for leg circulation.
Stretch and Breathe
Set a reminder to pause every hour. Stand up, stretch, and take 60 seconds of deep, slow, diaphragmatic breaths. This actively lowers your heart rate and signals the stress response to turn off.
Elevate Your Legs
At the end of a stressful day, lie down and elevate your legs above heart level for 15 minutes. This immediately eases pressure and helps pooled blood return to the core circulation.
Compression Therapy
Compression stockings offer a gentle, constant hug to your lower legs. They can reduce swelling and help your vein valves prevent backward blood flow. Consider wearing them on your most stressful, long work days.
Nutrient-Rich Foods
A healthy diet reduces systemic inflammation, which is directly linked to chronic stress. Focus on high-fiber foods and antioxidants to support strong blood vessels.
Weight Management
Obesity is a major risk factor for the progression of chronic venous insufficiency. Even modest weight loss can improve symptoms and venous pressure.

Your Action Plan for Better Vein Health
Here are 10 simple, actionable steps you can take today (and continue to practice) to lower your stress level and boost your leg vein health:
- Practice Mindfulness: Focus on breathing and being in the moment.
- Take a Quick Walk: A 10-minute walk around the office or block can lower your stress.
- Hydrate: Remember to drink water throughout the day.
- Leg and Ankle Stretches: Do 10 calf raises or ankle circles.
- Limit Screen Time: Put down your phone or close your laptop 30 minutes before bed.
- Find a Hobby: Engage in a non-work activity for 20 minutes (reading, music, or a puzzle).
- Connect with Nature: Step outside and focus on the sights, sounds, and smells of the natural world.
- Get 7+ Hours of Sleep: Prioritize good sleep to destress and recharge.
- Reach Out: Make an effort to reconnect with a friend or loved one. Even a text or phone call can make you feel more relaxed.
- Schedule an Expert Check-in: Book a free consultation with a vein specialist for your peace of mind.

Stress and The Power of Proactive Care
Stress is an unavoidable part of modern life, but its impact on your leg vein health doesn't have to be. By understanding the connection, you can be empowered to make simple, but powerful lifestyle changes to maintain your long-term vein health. Take control of your vascular health today by scheduling a consultation with a vein specialist at Metro Vein Centers. Your legs are worth it!
Frequently Asked Questions
Chronic stress indirectly contributes to varicose veins by causing repeated spikes in blood pressure and inflammation, which weaken vein walls and damage the tiny valves inside. When valves fail, blood pools, causing veins to swell and twist, which can lead directly to varicose veins.
Yes, chronic stress can significantly increase your risk factors for Deep Vein Thrombosis (DVT), but stress itself doesn’t directly create a clot. High cortisol levels and elevated blood pressure can inflame the lining of veins and thicken the blood. When combined with stress-related inactivity, these changes can create an environment where blood clots are much more likely to form.
Yes, chronic stress can significantly impair leg circulation. When stressed, your body releases cortisol and adrenaline, which cause blood vessels to constrict and blood pressure to rise, making it harder for blood to flow back to the heart. Incorporating low-impact exercises like walking or ankle pumps can help manually stimulate circulation and counteract these stress-induced vascular changes.
You should consult a vein specialist as soon as you notice persistent symptoms, such as leg heaviness and visible veins. If leg heaviness, aching, swelling, or the appearance of new visible veins (spider or varicose) last for more than a few weeks, it’s time for a vein health assessment to rule out venous disease.
Stress-related habits increase the risk of vein disease. A poor diet can cause inflammation and weight gain, which can increase pressure on leg veins. Sedentary behavior negatively impacts circulation. Poor sleep can prevent the body from repairing damaged blood vessels and controlling inflammation. Stress management, however, is an essential step in protecting your vein health.

Dr. Philip LoPresti
Meet Dr. Philip LoPresti DO, DABVLM, FACS, a board-certified vein specialist and surgeon with over 20 years of experience. Schedule an appointment with him in Queens, NY today.
Meet Dr. Philip LoPresti
Trusted insight from the nationally accredited, board-certified vein doctors at Metro Vein Centers.