Legs can swell for a variety of reasons, from diet and lifestyle to deeper, medical concerns beneath the surface of the skin. It may seem like an everyday, unavoidable experience, but there are surefire ways to reduce swelling in the legs or even eliminate leg swelling entirely. Swelling in the legs is one of the most common symptoms of chronic venous insufficiency (CVI) and related poor circulation issues, with the majority of people with this condition reporting or experiencing swelling in their calves, feet, and ankles (oftentimes experiencing leg swelling when flying in airplanes) when they come in for evaluation with our team of vein specialists. But why do legs swell, and what does that have to do with our veins? Keep reading; we’ve got you covered.
Understanding the Causes of Leg Swelling
Leg swelling, or edema, is a common condition characterized by the visible accumulation of fluid in the extremities, typically occurring beneath the pelvis in the thighs, calves, ankles, and feet. In fact, one of the early warning signs of leg swelling is noticed in the ankles: if you remove your socks and see a ring around your ankle, you may be experiencing leg swelling! This condition stems from a range of underlying factors, with impaired blood circulation playing a central role. Veins in the lower limbs bear a substantial responsibility within the circulatory system, tasked with returning blood to the heart against the pressure of gravity. Over time, these veins can weaken from all that work, leading to valve dysfunction. Veins are meant to pump blood one way (back to your heart), but when these valves malfunction blood tends to pool and flow backward, causing an excess buildup of fluid in the legs, thus resulting in swelling.
For individuals already experiencing swelling due to poor circulation, certain factors can exacerbate their discomfort, including but not limited to:
1. Prolonged inactivity: Lack of physical movement, whether from extended periods of sitting or standing (such as at work), can worsen swelling. Insufficient calf muscle contractions during prolonged immobility can impede the effective flow of blood (which is why it’s recommended to walk the aisles periodically on airplanes!).
2. Sodium intake: Elevated sodium levels in the body can lead to fluid retention. If you regularly consume salty foods and experience swelling, see if cutting some of the sodium from your diet reduces the swelling in your legs!
3. Dehydration: Inadequate hydration can lead to thicker blood, hindering circulation and potentially contributing to leg swelling/edema. When your veins have to work harder to pump your blood, valves can become damaged. The more water you drink, the smoother your blood flow will be.

4. Pre-existing vein issues: Individuals with pre-existing vein conditions, such as varicose veins in the legs, may experience leg swelling. Varicose veins already have impaired blood flow, causing or adding to swelling in the legs.
Additionally, one seasonal and environmental factor that may be worsening swelling in the legs is heat. Heat edema causes (or aggravates) swelling in the legs due to the body’s survival instinct to retain water in arid or hot environments. If you notice your legs swelling in the heat, cold compresses and leg elevation can help to alleviate heat edema or any swelling in the legs that comes on with higher temperatures.
It’s important to recognize that severe or persistent leg swelling might indicate an underlying medical issue, such as chronic venous insufficiency, poor circulation, or varicose veins. If your symptoms are not alleviated with lifestyle adjustments, it may be time to consult with a medical professional to discuss lasting, meaningful relief to your uncomfortable swelling.
If you notice asymmetrical swelling (one leg but not the other) accompanied by tender skin, very warm/flushed skin, and/or skin hardness, we recommend seeking urgent care, as these may be the signs of a blood clot in your deep veins.
Do Varicose Veins Cause Leg Swelling?
Varicose veins can cause edema (swelling) in the legs. When varicose veins develop, blood flow is impaired, leading to fluid buildup in the surrounding tissues. This venous insufficiency often results in swelling, particularly in the ankles and lower legs, as a common symptom of varicose veins.
Managing Leg Swelling: Strategies for Relief
You may be able to manage and reduce swelling in the legs on your own! It’s important to note, however, that if your symptoms persist or worsen, you may need to seek out additional measures to achieve relief. These lifestyle changes, while small, may improve the swelling and discomfort in your legs. Here’s a multifaceted approach that addresses underlying causes and promotes healthy circulation:
1. Stay hydrated: As mentioned above, adequate hydration helps maintain a generally healthy fluid balance in the body, so consistently drinking enough water throughout the day supports smooth blood flow by making it easier for your veins to move blood efficiently. Edema can be reduced with an intake of 2.5 – 3.5 liters of water per day (8 full cups of water). Also avoid consuming large amounts of dehydrating beverages like caffeine and alcohol.
2. Take movement breaks: Avoid prolonged periods of inactivity, as sedentary lifestyles can inhibit healthy circulation. Take advantage of breaks at work to move around and stretch your calves. Any low-impact exercise can also help promote good circulation in the entire body without putting too much strain on your legs or joints. Even simple calf raises (which contract your leg muscles) while you brush your teeth can improve circulation in your lower extremities.
3. Elevate your legs: Resting your legs above the level of your heart can help reduce swelling by encouraging blood flow in the right direction (back towards your heart). Gravity inhibits blood flow, so reversing that sometimes with simple elevation can provide drastic improvement.
(If swelling is reduced by leg elevation alone, your edema is most likely caused by vein disease. Poor circulation is the root cause of most varicose vein symptoms and discomfort.)
4. Wear compression garments: Graduated long compression stockings (over the knee) can enhance circulation by applying gentle pressure that encourages blood flow from the legs back to the heart. These can be worn beneath pants and long skirts or dresses. We recommend 30 mmHg of pressure, and we advise our patients to remove their compression stockings before going to sleep for the night.
5. Cool compresses: Heat can aggravate swelling, as hot weather can actually cause the body to retain moisture. Applying cool compresses to swollen areas can help reduce inflammation and remind the body that you are not, in fact, wandering aimlessly through a sandstorm. Literally “chilling out” helps blood vessels begin to dilate again, allowing blood to flow uninhibited, and providing relief from swelling. Goodbye, heat edema!
6. Massage: Gentle, upward-moving massages can promote lymphatic drainage and improve circulation. Move with the flow of your blood, from ankle to knee, and be sure to apply some oil or lotion to add slip and help reduce strain on your skin. Avoid excessive pressure on swollen areas, and do not continue if you experience pain.

7. Monitor sodium intake: As we mentioned before, excessive salt consumption can lead to fluid retention and exacerbate swelling. Reducing sodium intake can encourage your body to stop holding water.
8. Maintain a balanced diet: Incorporate potassium-rich foods, such as bananas, spinach, and avocados into your meals, as potassium helps regulate fluid balance. Adding iron-rich foods or supplements to your daily intake can also help with circulation.
9. Seek medical consultation: If your leg swelling is severe, painful, or persistent, or if it is accompanied by other concerning symptoms such as restless legs, aching, tingling, or burning, we recommend consulting a board-certified vein doctor and seeking permanent solutions.
Seeking Relief
Swelling in the legs is not uncommon, and while it can be due to a variety of factors, from diet and exercise habits to temperature and even pregnancy, swelling in the calves, ankles, and feet can often be attributed to poor circulation as a result of vein disease. Vein disease is progressive, which means it will worsen over time if left untreated, so it’s important to keep track of symptoms if they are becoming more difficult to handle. If your minor swelling has increased, or if your swelling is accompanied by painful symptoms, it’s best to get a leg up on vein disease (and, again, we mean literally elevate those legs) by seeking the opinion of a board-certified vein specialist.
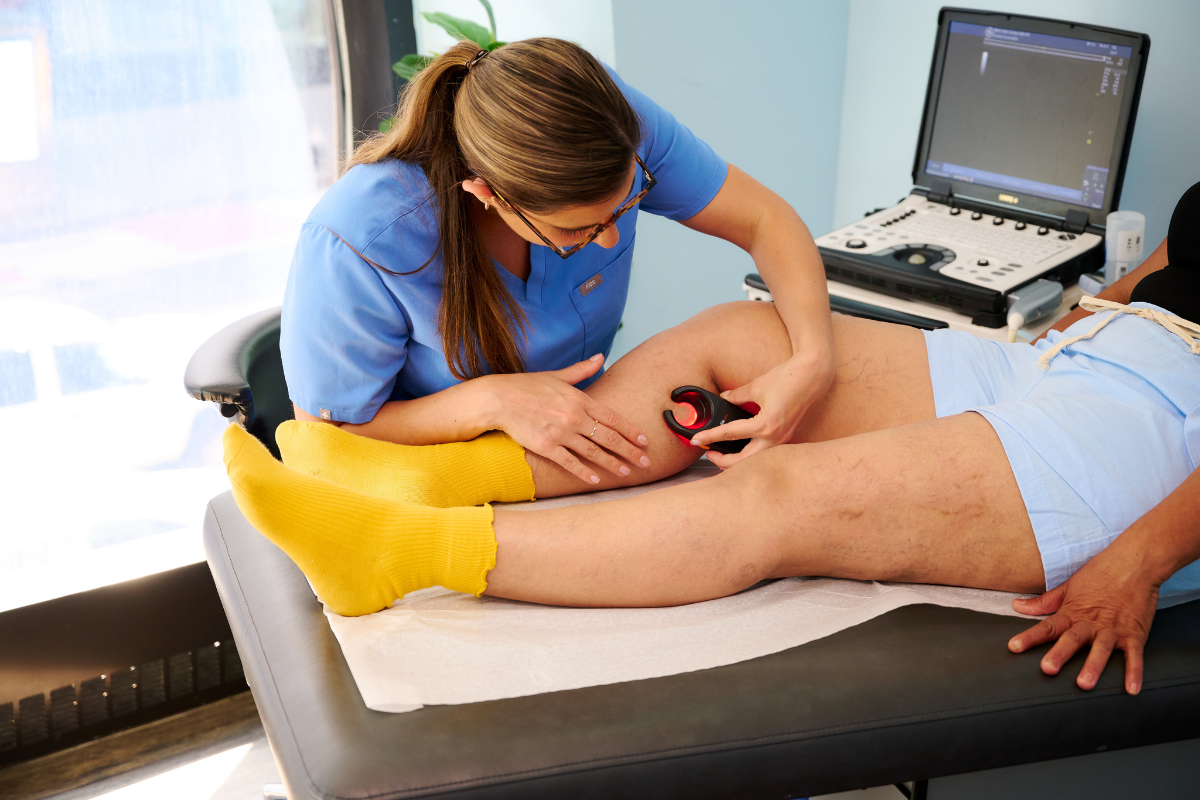
At Metro Vein Centers, we offer free vein evaluations in all of our clinics. You will discuss your leg swelling and any other concerns with a vein doctor directly. We may recommend an additional ultrasound to investigate the presence of deep vein thrombosis (DVT) or varicose veins beneath the surface of the skin. Although many cases of varicose veins are visible to the naked eye as bulging or twisted blue, green, red, or purple veins, deeper veins in the legs can also become varicosed — the only difference is that they cannot press against the skin and so are not visible.
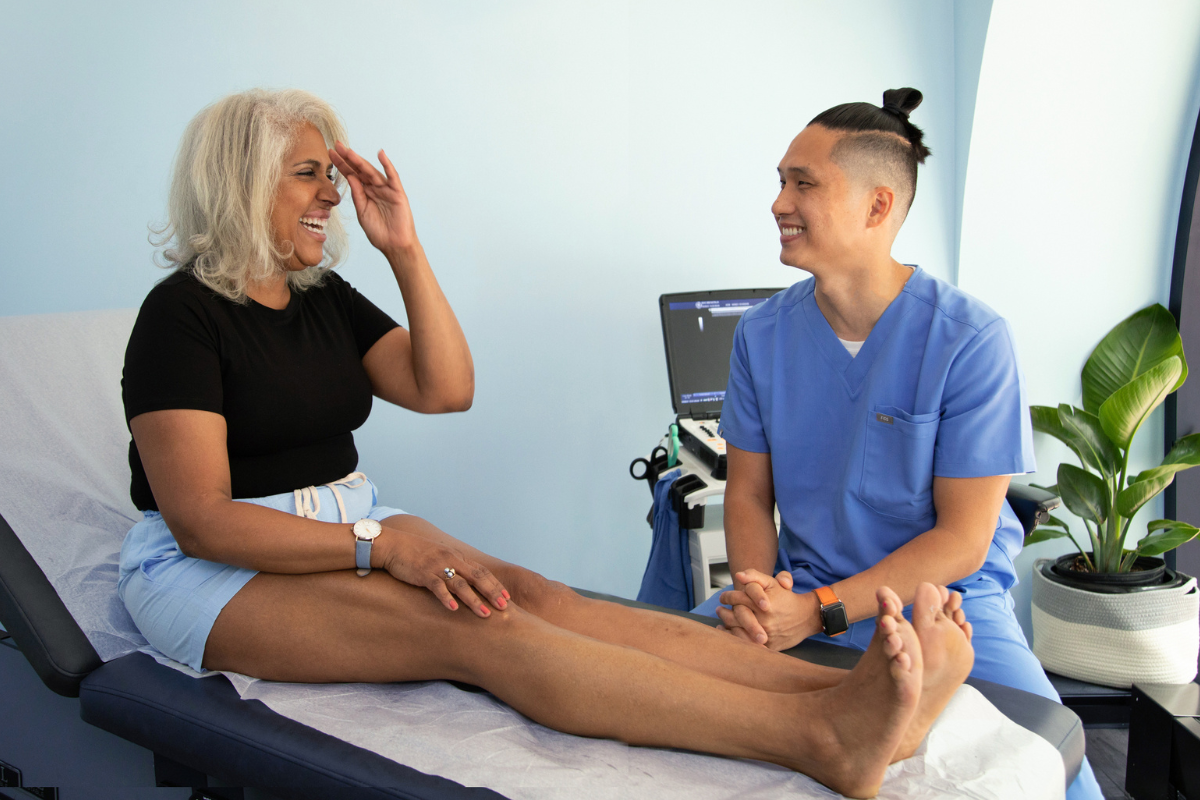
While swelling, aka edema, is a common symptom of vein diseases like chronic venous insufficiency, DVT, and varicose veins, that does not mean it is unavoidable or untreatable. We offer a variety of FDA-approved, minimally invasive vein treatment options that can remedy vein disease at the source, which in turn will eliminate painful or uncomfortable symptoms. If your pre-existing swelling is becoming frustrating, we recommend coming in for a free vein evaluation in any of our New York, New Jersey, Connecticut, Michigan, or Texas vein clinics. Poor circulation, swelling in the legs, ankles and feet, varicose veins, and vein disease all can be remedied with minimally invasive, FDA-approved vein treatment options. Our vein specialists are here to help! Give us a call at 866-353-6303 to schedule your free vein evaluation and look forward to enjoying summers again!
Metro Vein Centers Editorial Team
From vein care 101 to treatments, the Metro Vein Centers blog offers patients everything they need to know about vein health.

Trusted insight from the nationally accredited, board-certified vein doctors at Metro Vein Centers.